There are basically 2 types of shoulder replacement.
- Anatomical shoulder replacement
- Reverse total shoulder replacement
The age, activity, the kind of shoulder disease, stage of disease and whether the
rotator cuff is intact and healthy or not dictate the kind of shoulder replacement the
patient needs.Our doctor is one of the top Shoulder replacement surgeon in Surat. He has experience of handeling complicated shoulder replacement surgeries.
1. What is shoulder arthritis?
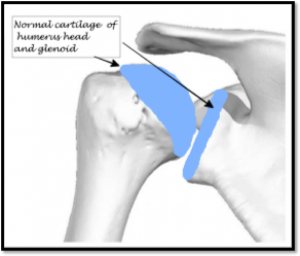
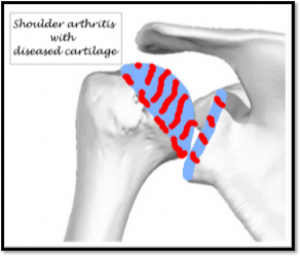
Cartilage is the protective covering over the opposing surface of bones, which form a
joint. They facilitate smooth and painless movement of both the bones on each other.
When this cartilage cover is completely lost and there is pain on movement of the
joint it is called as arthritis.
2. What is the cause of arthritis?
Arthritis may be due to various causes.
- Age related: In elderly patients due to wear and tear over the years the cartilage
gets damaged and there is arthritis
- Rheumatoid arthritis, Psoriatic arthritis etc.: In patients with long standing
rheumatoid arthritis, psoriasis, gout and other diseases which affect the joints;
the shoulder joint can also get involved leading to arthritis
- Post infection: Sometimes shoulder arthritis may be seen long after a infection in
the shoulder joint has occurred and has been cured. Patients have pain; which starts
slowly and progressively increases in severity
- Post traumatic: Similarly in many patients arthritis may set in after a shoulder
injury many years back or some shoulder surgery for fracture months or years back.
- Avascular necrosis humerus head: This is a condition in which the bone under the
cartilage of the head of humerus collapses due to loss of blood supply and death of
the bone. Eventually the smooth surface of the cartilage becomes rough and arthritis
sets in. It may happen in patients with fracture, after surgery for fracture of
head, in patients with sickle cell disease or rarely after deep-sea diving or high
mountain climbing.
- Rotator cuff arthropathy: In patients
3. What are the symptoms of arthritis?
Pain and difficulty in movement of the shoulder are the initial symptoms. Patients
have difficulty in sleeping on the affected side. Sleep disturbance, inability to lift
hand above face level, grating sensation in the shoulder are seen in later stages.
4.What is the treatment for Shoulder arthritis?
If rest, activity modification and physiotherapy do not help then the only option for
clinically significant arthritis is shoulder replacement. There are 2 types of
shoulder replacement: anatomic shoulder replacement and reverse shoulder replacement.
Anatomic Shoulder replacement
Here the spherical structure of the head and cup structure of glenoid is kept intact
and the diseased cartilage and bone is replaced with metallic surfaces. This removes
the pain generating cause from the shoulder and gives relief to the patient.
Reverse shoulder replacement
Here the diseased cartilage and bone is removed and the spherical structure of the
head is converted into a cup and the glenoid has a globular shape. This is needed in
patients with arthritis due to rotator cuff arthropathy. Because of the unique design
of this replacement prosthesis patients who are initially not able to lift their arms
are able to lift their arms overhead, able to do their daily activities and pain is
almost completely gone.
5. What is the hospital stay? What is the recovery period? Do I need bed
rest?
The hospital stay is of 2-3 days. Recovery period varies from patient to patient.
Please ask the doctor during consultation about the details. No bed rest is needed.
Patients start moving and are independent the same day after surgery.
6. What is the age limit to undergo this surgery? What if I have diabetes,
hypertension or thyroid disorders?
As such there is no age limit. Every patient needs to be evaluated individually.
Patients who are active and their lifestyle is disturbed due the shoulder arthritis
need this surgery. Medical diseases if present have to managed properly before, during
and after surgery. Otherwise patients who are deemed fit by the anesthetist can
undergo this surgery and have a good result. Still any query book your appoinment with best shoulder arthroscopy surgeon of Surat, Our doctor will consult & solve your queries.






